The Diagnostic Pathway
NEW
See expert guidelines on diagnosis and management strategies
Consider PK deficiency in all patients displaying lifelong chronic hemolysis where other causes have been excluded1-3
A definitive diagnosis of PK deficiency is essential for monitoring and management decisions
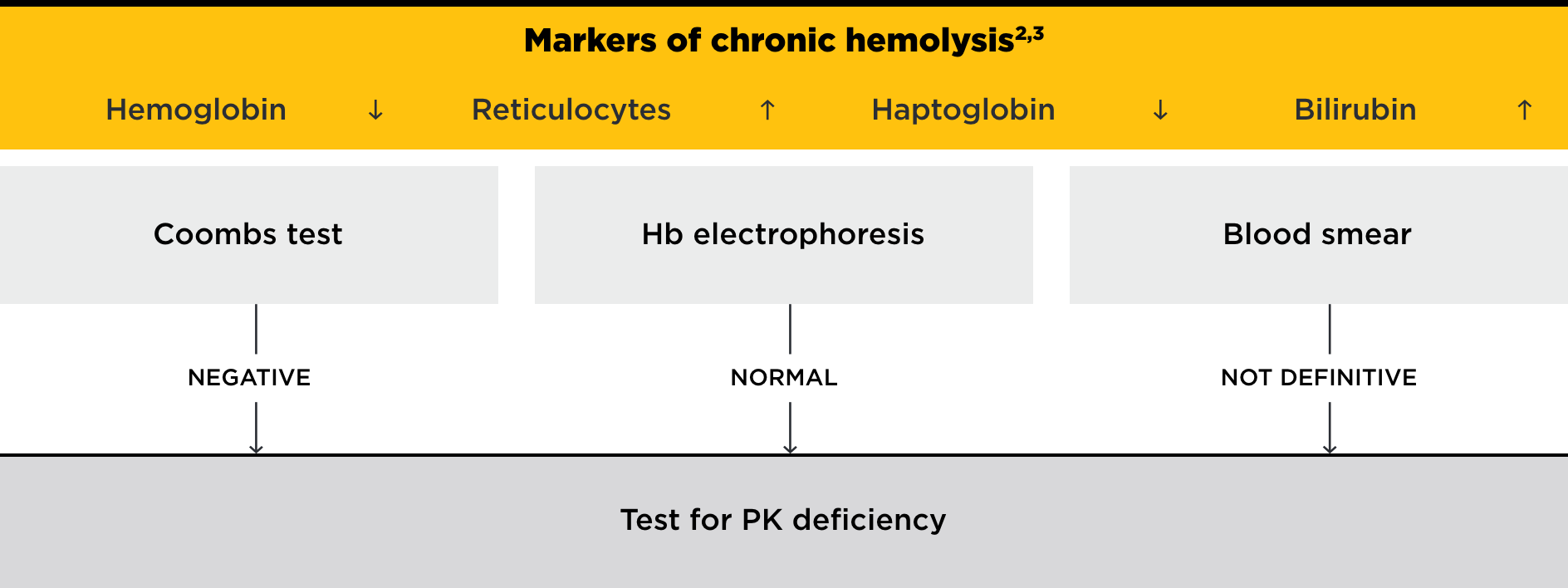
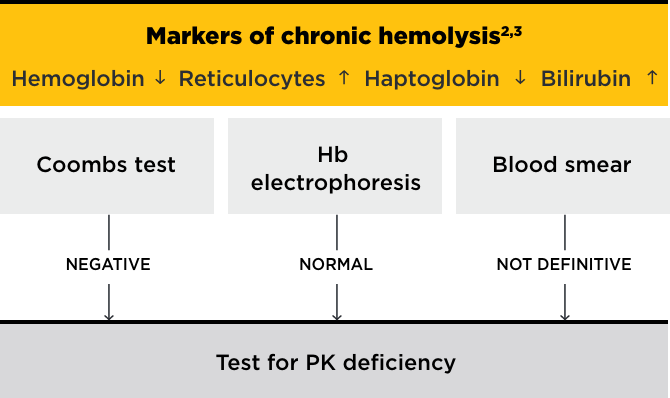
Differential diagnosis4,5
Hematologic features of PK deficiency are not specific and can overlap with other diseases, including:
- Autoimmune hemolytic anemias
- RBC membranopathies
- Other RBC enzymopathies
- Hemoglobinopathies
Case Profile*: Delayed Diagnosis2
Baseline hemoglobin (Hb) improvement of 11.5 to 12.5 g/dL
- Hb: 10.9 g/dL (low)
- Absolute reticulocyte count:
1030 × 109/L (high) - Haptoglobin: undetectable
- Indirect bilirubin: 3.7 mg/dL (high)
- Direct antiglobulin test: negative
- Hb electrophoresis: unremarkable
- Erythrocyte membrane defects: negative
PK activity: 1.2 U/g Hb (reference range, 6.7-14.3 U/g Hb)
Compound heterozygosity for 2 PKLR missense mutations
*Due to the variability of the disease, case profiles are not reflective of every patient.
References: 1. Bianchi P, Fermo E, Glader B, et al. Addressing the diagnostic gaps in pyruvate kinase deficiency: consensus recommendations on the diagnosis of pyruvate kinase deficiency. Am J Hematol. 2019;94(1):149-161 [supplementary online material]. 2. Al-Samkari H, van Beers EJ, Kuo KHM, et al. The variable manifestations of disease in pyruvate kinase deficiency and their management. Haematologica. 2020;105(9):2229-2239. 3. Grace RF, Layton DM, Barcellini W. How we manage patients with pyruvate kinase deficiency. Br J Haematol. 2019;184(5):721-734. 4. Grace RF, Zanella A, Neufeld EJ, et al. Erythrocyte pyruvate kinase deficiency: 2015 status report. Am J Hematol. 2015;90(9):825-830. 5. Nassin ML, Lapping-Carr G, de Jong JLO. Anemia in the neonate: the differential diagnosis and treatment. Pediatr Ann. 2015;44(7):e159-e163.